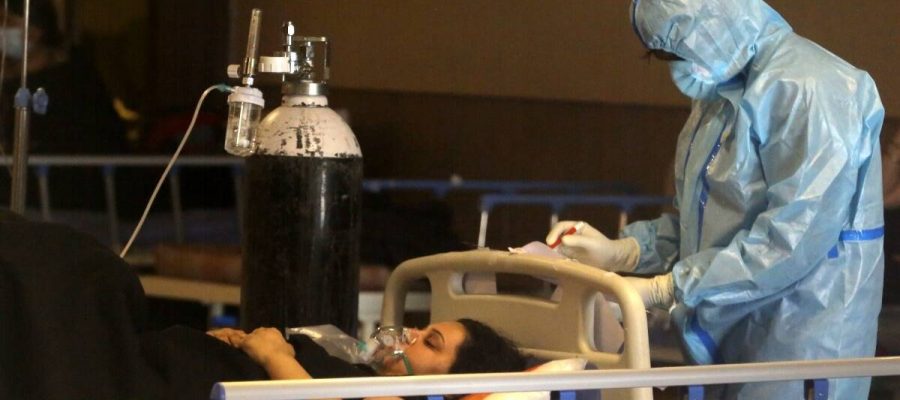
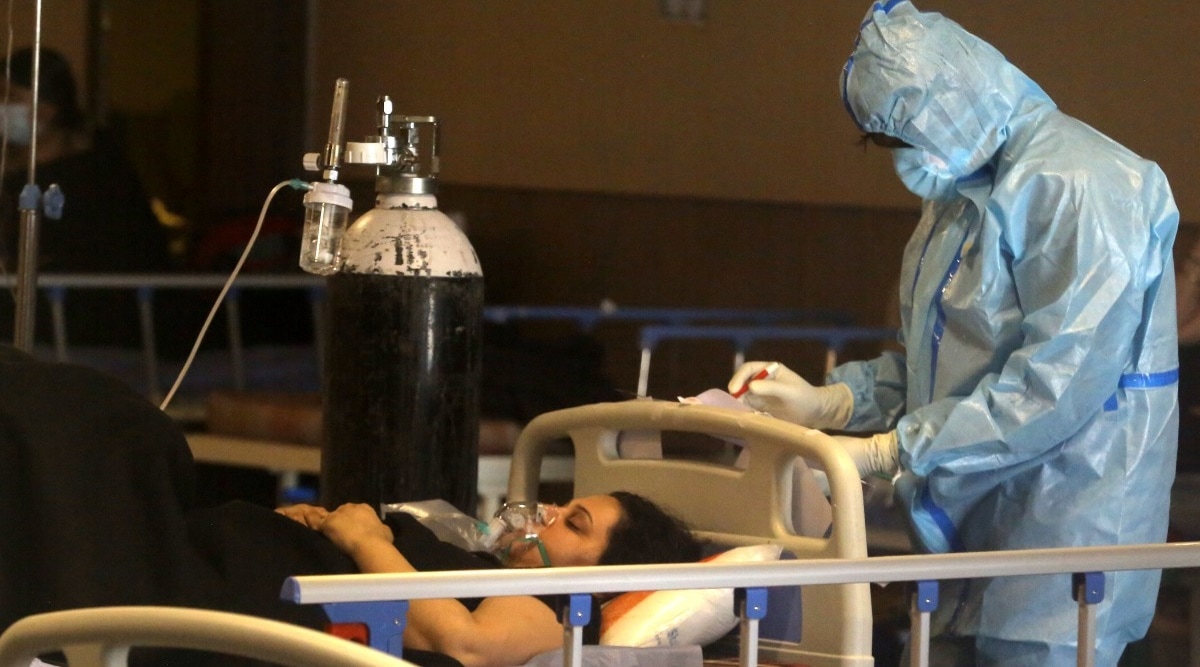
Doctors are consciously limiting early use of steroids in patients to reduce the chances of secondary infections, and advise patients not to start steroids at home.
NOT JUST mucormycosis, but other fungal infections such as candidiasis and aspergillosis have become increasingly common among intensive care units and Covid-recovered patients. Doctors are consciously limiting early use of steroids in patients to reduce the chances of secondary infections, and advise patients not to start steroids at home.
On Sunday, the state task force held two meetings – one with 700 general practitioners (GPs) in Mumbai and Thane, and the second one, with chest physicians. The GPs were advised on following treatment protocol and using steroid only in patients whose oxygen saturation drops or in those who suffer inflammation and require ICU.
Mucormycosis is caused by mucormycetes that generally attacks a diabetic person with low immunity. For a year, even normally healthy patients are reporting this infection post Covid. The infection can pass through the environment, contaminated oxygen pipe or from ICU into a patient.
Most report headaches as early signs within two-four weeks of recovery from Covid. If delayed, it can travel upwards into the brain and be fatal. Candidiasis, on the other hand, is not life threatening, it spreads through candida fungus and is common in ICU Covid-19 patients. It infects the throat, mouth, gut but is easily treatable.
Aspergillosis infection spreads in the respiratory tract and lungs. Doctors are reporting this infection in Covid-19 patients with low immunity, and in cases with high steroid use.
“Steroids must be used in low doses in patients, who need oxygen and only after second week of Covid infection starts. Steroids must be used for 7-10 days,” said Internal Medicine Specialist Dr Paritosh Baghel from SL Raheja Hospital. “We are noticing that patients are buying it over the counter and taking steroids at home and in smaller nursing homes, doctors are administering it in high doses,” he added.
Baghel said only in rare cases, where inflammation does not settle, a doctor takes a call to use steroids like Dexamethasone and Methylprednisolone beyond 10 days. Consultant Dr Shahid Barmare, who has seen five such cases in the past two weeks, said doctors have become cautious and refrain from prescribing steroids for mild and asymptomatic patients.
Dr Kedar Toraskar, critical care specialist in Wockhardt Hospital, said the task force has advised to stop steroid use when patients get clinically well. “It is not to be administered at home without a doctor’s prescription. Mucormycosis is the most common fungal infection in Covid-19 patients and in most cases, diabetic patients are getting it. We are also seeing a lot of aspergillosis cases,” he said.
Dermatologist Dr Nitin Nadkarni said the ICMR treatment protocol is streamlined and needs no modification. “We just need doctors to follow it. High dosage of steroids compromises immunity, making patients susceptible to fungal infection.” He added that in some cases, the infection can get fatal and affect the brain if not treated on time.
Dr T P Lahane, director of Directorate of Medical Education and Research in state, reported death of eight Covid-recovered patients due to mucormycosis. Common symptoms of mucormycosis are headache, blocked nose, foul discharge or bleeding from nose and redness of eyes.
Source: Read Full Article